If you’ve spent your life believing that eating disorders have a specific “look,” you aren’t alone. There’s a reason that the SWAG (skinny, white, affluent girl) stereotype — an unfortunate artifact of early research on patients with anorexia nervosa — is still so dominant.
But eating disorders don’t discriminate.
Not only can people of all ages, genders and races struggle with anorexia, so can people of all weights. Unfortunately, society — and even some medical professionals — have reinforced the myth that you have to be underweight to be “sick enough” to need help for a restrictive eating disorder.
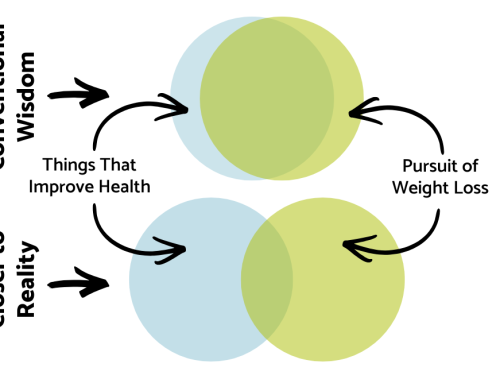
But here is the hard, clinical truth: You cannot determine someone’s health, or their relationship with food, by looking at the size of their body. It’s the behaviors and mindsets, not body size, that matters.
As an eating disorder specialist, I’ve had many clients in average-to-higher weight bodies who came to me trapped in a cycle of severe food restriction, intense fear of weight gain, and obsessive food thoughts. In spite of that, they tell me, “I don’t have a problem…I just need to lose weight,” when really they have atypical anorexia.

What is atypical anorexia? (OSFED explained)
The word “atypical” is a bit of a misnomer. In clinical settings, we use the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) to categorize illnesses. Atypical anorexia isn’t grouped with “typical” anorexia. falls under the umbrella of OSFED (Other Specified Feeding or Eating Disorder).
Someone with atypical anorexia meets every single diagnostic criterion for anorexia nervosa — the food restriction, the intense fear of gaining weight, and negative body image — except they don’t have an “underweight” BMI. Instead, they have a BMI in the “normal,” “overweight,” or “obese” range.
The irony? There is nothing “atypical” about the suffering. Research shows that the medical and psychological complications of atypical anorexia — such as heart rate instability, electrolyte imbalances, fainting, and suicidal ideation — are just as severe as those seen in patients with low body weights.
As one eating disorder researcher once told me, people with atypical anorexia have greater body image disturbance, whereas typical anorexia may have more medical complications. However, both groups show the hallmarks of malnutrition: loss of periods, bone loss, orthostatic hypotension (an abrupt drop in blood pressure when someone stands up) and electrolyte imbalances.
The ‘wellness’ mask: how society praises eating disorders in larger bodies
The most dangerous thing about atypical anorexia is that it is often socially reinforced. When a person in a larger body begins to restrict food or over-exercise, they are often praised. They hear:
- “You look great! What’s your secret?”
- “I wish I had your willpower.”
- “Keep up the hard work.”
For the person suffering, these “compliments” act like fuel for the eating disorder. They validate the internal voice that says hunger is a weakness and that their worth is tied to making their body smaller. Because they’re being congratulated for their symptoms, they rarely recognize that they are actually in a medical crisis.
When someone with anorexia is underweight, their healthcare providers tell them they need to eat more and gain weight, and that gaining weight is OK. Sadly, the opposite is true when the person is “overweight.” They get the message from the professionals they are trusting with their health that they eat too much and weigh too much. Again, that totally plays into their eating disorder.
Someone with atypical anorexia may be fainting or having pain from low gastrointestinal motility — a common side effect of severe caloric restriction or weight loss — but they’re not treated the way they would be if they were underweight. Instead, they’re treated like they’re eating too much.

The myth of ‘just needing to lose weight’
If what I’ve written so far sort of describes you, but you’re thinking “I’ll stop these behaviors once I reach my goal weight,” I want you to pause for a moment.
In the mindset of eating disorders, the goalpost always moves. The “goal weight” is a mirage. Once you reach it, the eating disorder will tell you it wasn’t enough weight, or that you had to restrict even more to make sure you don’t gain it back.
When you believe you “just need to lose weight,” you are often experiencing internalized weight bias. This is the belief that a smaller body is inherently healthier or more valuable. You may also wish to escape weight bias directed at you from others. However, if the path to a smaller body involves malnutrition, obsessive thoughts, and the loss of your social life, it is not “health.” It is a slow-motion collapse of your well-being.
We should all be concerned about overly controlled, restrictive, obsessive food thoughts and behaviors — in ourselves and others. That’s where we need to draw a line.
In our society it can look “healthy” to be really obsessive, but if all you talk and think about is weight and body and food, that’s not a balanced healthy life. The cost on your relationships and your quality of life is too high.
The physical toll is real: atypical anorexia symptoms
Like it or not, your heart, brain, and bones do not care what the scale says — they only care if they are being fueled. When you restrict your intake, your body enters a state of semi-starvation.
Even if you are in a larger body, your metabolism will slow down to conserve energy, and you might experience:
- Bradycardia: A dangerously low heart rate.
- Orthostatic hypotension: Feeling dizzy or blacking out when you stand up.
- Amenorrhea: The loss of your menstrual cycle (yes, this can happen at any weight).
- Gastroparesis: A slowing of the digestive system that causes bloating and pain.
If you’re experiencing these things, you are not ‘failing’ at a diet. You don’t need to work harder. You’re experiencing the physiological consequences of an eating disorder.
Research shows that medical complications from severe calorie restriction can be serious at any body weight, and has found that weight suppression itself — the difference between a person’s highest and current weights — drives severity of symptoms.

Why believing you aren’t ‘sick enough’ is a trap
The myth that anorexia “doesn’t happen’ in people in larger bodies is extremely harmful. The most common reason people with atypical anorexia don’t seek help is that they don’t believe they’re “sick enough.” They may think they’re just doing what they’re supposed to restrict calories and lose weight in order to be healthy. They delay seeking help until they hit a certain weight or until they collapse.
Eating disorders are never healthy, and you do not need to earn your recovery. The severity of an eating disorder is measured by the degree of your mental obsession and the impact on your life, not your BMI. If food has become your primary preoccupation, if you feel guilt every time you eat, and if your “health journey” has robbed you of your joy — you are sick enough right now.
How to start the healing process with a HAES dietitian
Recovery from atypical anorexia requires a weight-inclusive approach. This means working with a team (therapist, dietitian, and doctor) who understands that health is not about a particular body size and that weight loss is not a valid treatment for an eating disorder.
Some initial steps are to:
- Acknowledge the pain: Admit that the restrictive mindsets and eating behaviors has become a prison.
- Seek specialists: Look for providers who are weight-inclusive, HAES (Health at Every Size)-aligned.
- Challenge the praise: Start to recognize that external compliments on your weight loss are triggers for your eating disorder.
- Focus on re-feeding: The first step in eating disorder recovery is always consistent, adequate nourishment — no matter your size. Your brain cannot heal if it is starving.
If you have been told your whole life that your body is a problem to be solved, it is incredibly brave to decide to stop fighting against it. You deserve to take up space. You deserve to eat without a side of shame. And most importantly, you deserve medical care that sees your struggle, not just your BMI. If you’re thinking about seeking help, feel free to reach out. Just click here to schedule a free 20-minute Discovery Call to talk about your concerns and see if we’re a good fit.

Disclaimer: All information provided here is of a general nature and is furnished only for educational purposes. This information is not to be taken as medical or other health advice pertaining to an individual’s specific health or medical condition. You agree that the use of this information is at your own risk.
Hi, I’m Carrie Dennett, MPH, RDN, a weight-inclusive registered dietitian, nutrition therapist and body image counselor. I offer compassionate, individualized care for adolescents adults of all ages, shapes, sizes and genders who want to heal from an eating disorder, disordered eating or chronic dieting, cultivate an accepting, respectful relationship with their bodies, and gain the freedom to live an authentic, meaningful life without obsessing about food.
Need 1-on-1 help for your nutrition, eating, or body image concerns? Schedule a free 20-minute Discovery Call to talk about how I can help you and explore if we’re a good fit! I’m in-network with Regence BCBS, FirstChoice Health, Providence of Oregon Health Plan and United Healthcare, and can bill Blue Cross and/or Blue Shield insurances in many states. If I don’t take your insurance, I can help you seek reimbursement on your own. To learn more, explore my insurance and services areas page.
 Print This Post
Print This Post