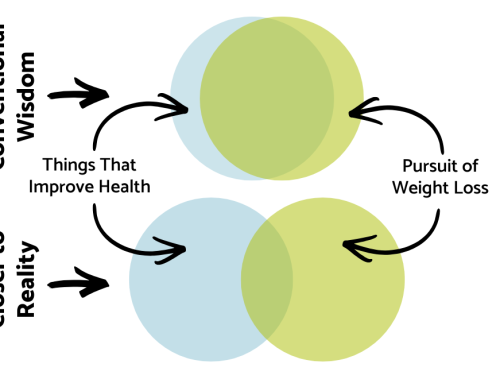
Trigger Warning (TW): This posts mentions the “O” words numerous times.
The subject matter of this post falls under the heading of surprising/not surprising, I think. For me, hearing the information I’m about to share with you clarified some things I already knew because it lined up the details neatly. Namely, Big Pharma’s culpability in the so-called “obesity epidemic.”
Last week, I spent a very satisfying morning attending a virtual weight-inclusive public health symposium put on by the University of California, Berkeley, School of Public Health. To my great delight, the first speaker was Katherine Flegal, an epidemiologist and senior scientist at the Centers for Disease Control and Prevention (CDC).
If you subscribe to my newsletter, you may remember that I wrote a bit about Flegal a few months back, specifically referencing very solid 2005 and 2013 research papers she co-authored in the Journal of the American Medical Association, which found that being “overweight” was associated with lower mortality rates than being “normal weight.”
I also wrote about how those papers really twisted the knickers of white male-dominated public health institutions, and how they went after her with a vengeance. You can learn more about that specifically in the 2021 paper (“The obesity wars and the education of a researcher: A personal account”) Flegal wrote about her experience, and in an excellent episode (“Is being fat bad for you?”) of the “Maintenance Phase” podcast. (She also has a new article in Annual Review of Nutrition about her career as a woman in research, which also addresses the knicker twisting).

The emerging weight loss drug market
Back to Flegal’s recent talk, which started with the blunt statement that the medicalization of body size (the so-called “obesity epidemic,”) was largely a product of efforts to promote weight loss drugs. Anti-fatness and weight stigma may be an incidental result of these marketing attempts. In other words, collateral damage.
Flegal pointed out that a lot of language about weight today is sensationalist, with “obesity” is portrayed as the most prevalent health problem. However, prior to the late 20th century “overweight” and “obesity” were not considered a population-wide health risk. Research in the 1970s and 1980s found that BMI was not related to cardiovascular disease once they considered other factors.
Then, in the 1990s came a transition to the use of prescription weight loss drugs for long-term treatment of “obesity.” First came Fen-Phen in 1992. In 1995, the Food and Drug Administration approved dexfenfluramine (Redux), and just 3 months later, doctors were writing 85,000 prescriptions a week. Flegal said one securities analyst projected that sales of Redux would hit $1 billion in 5 years. That projection never came to pass, because the Redux and Fen-Phen were both withdrawn from the market in 1997 due to negative cardiovascular side effects. Sibutramine (Meridia), was approved in 1997 as a supposedly safer alternative to Fen-Phen and Redux, then withdrawn in 2010. Orlistat (Xenical) was approved by FDA in 1999 and is still around despite the fact that the side effects include gas with oily anal discharge, and urgent or hard-to-control bowel movements. Fun!

The medicalization of body size
A spokesman for the pharmaceutical company Roche said “part of our challenge moving forward with Xenical is to ‘medicalize’ weight management to physicians.” Why was it a “challenge”? Because weight loss was largely seen as a cosmetic issue, not as a health issue:
- The IRS would not allow weight loss treatment to be considered as a medical deduction for tax purposes.
- Weight loss drugs were relatively ineffective and had a checkered history.
- Health insurance did not cover weight loss treatments…and iff insurance doesn’t cover it, doctors aren’t going to be reimbursed for it.
Around that same time – in 1995 – the World Health Organization (WHO) published a report on body measures. The report was more than 400 pages long. It took two years to put together, involved dozens of scientists, and covered all ages and many topics. The report used BMI to define three grades of “overweight” (note: not “obesity”) and described the method used to establish cut-off points as largely arbitrary. They did define “obesity” as a degree of fat storage associated with clearly elevated health risks – but noted that there was a lack of scientific consensus on what this meant, exactly.
Enter the International Obesity Task Force (IOTF), which was set up as a charity in the UK in 1996 by professor Phillip James. By 2000, IOTF had 29 “obesity expert” members from 19 different countries. While this group was a stand-alone entity and not part of WHO, people commonly thought that the group was, in fact part of WHO. This of course gave it an unearned air of authority and prestige.
Lobbyists pushing “public health”
IOTF’s mission was to inform the worlds’ governments about the urgency of the “obesity” problem and to persuade them that the time to act was now. Yes, they were a lobbying group and, wait for it…they got their money from drug companies. In a 2013 interview with the UK newspaper The Guardian, James said drug companies gave him checks for about 200,000 British pounds at a time. (That’s roughly the equivalent of 412,000 U.S. dollars today.) James claims the drug companies didn’t ask him a to push any specific agenda, but it’s naïve to think that all that money didn’t influence his behavior.
Certainly, the drug companies would benefit from raised awareness of the “obesity problem,” because they needed to sell their weight loss product.
In a 2008 article published in the International Journal of Obesity, James wrote that the IOTF was established with the express purpose of having a special consultation with WHO that would be “solely devoted to obesity.” WHO was actually reluctant to have a consultation on obesity. It wasn’t part of its biennial plan, and WHO’s executive board hadn’t agreed to it. But the meeting happened, and a draft report written by IOTF became the official working document, with only minor revisions. This report had new BMI categories. BMI of 25-30 was now “pre-obese”
WHO took the unusual step of disseminating an interim version of the report in 1998. Then IOTF paid to have free copies sent to health ministers of all 192 UN countries and to any others who requested it. (Flegal said she received two copies even though she didn’t request them.) So, why release the report early if it was going to come out officially in a few years anyway?

Poof…you’re now “overweight”
Flegal said at the same time the WHO stuff was going on, the NIH National Heart, Lung and Blood Institute (NHLBI) committee was preparing new clinical guidelines for “overweight and obesity.” Four IOTF members (including the chair) were on that committee. Perhaps this why the WHO report came out early…to influence the NHBLI report.
The most significant result of these clinical guidelines was that the BMI cutoff for “overweight” was lowered from 27 (28 for men) to 25. So overnight, millions of people became “overweight,” at least according to the NIH. “Obesity” was now defined as BMI 30 or higher.
The NHLBI guidelines received criticism, including concern that the new guidelines left the door open for widespread use of diet drugs – and potentially for weight stigma. Among other concerns were that the guidelines didn’t take into account important ethnic differences in weight that had been observed (and debated) for years. Even former Surgeon General C. Everett Koop said broadening the definition of overweight “will confuse the public and the medical community. It needlessly stigmatizes millions of Americans and lacks a solid scientific rational.”
A 1999 New York Times article pointed out that the new “overweight” and “obesity” cut points provided the pharmaceutical industry with “a booming new market for diet pills for the obese, practically served to the companies on a silver platter by the government.” But who exactly ended up taking these drugs?
Data gathered from the National Health and Nutrition Examination Survey between 2013-2016 found that it’s not just people who have BMIs in the “overweight” or “obese” category who are trying to lose weight. More than 35 percent of women with BMIs in the “underweight” or “normal weight” categories tried to lose weight in the previous year, as shown in this graph:

Officially labeling “obesity” as a disease
Returning to our original timeline, IOTF was working hard to get the Centers for Medicare & Medicaid Services (CMS) to stop prohibiting coverage for obesity treatment. The Medicare Coverage Manual said quite clearly that “Obesity itself cannot be considered an illness… Program payment may not be made for treatment of obesity alone since this treatment is not reasonable and necessary for the diagnosis or treatment of illness or injury.” This is significant, because health insurance companies generally follow the lead of Medicare’s recommendations.
In 2001, someone who was a member of both IOTF and the CDC engineered a CDC meeting about including “obesity” treatment in healthcare benefit plans. In other words, about reimbursing healthcare providers for obesity treatment. CDC followed up by requesting that CMS remove the prohibitive language from the Medicare manual, which CMS did in 2004.
Then, in 2013 the American Medical Association recognized “obesity” as a chronic disease. This flouted the recommendations of its Committee on Science and Public Health that “obesity” should not be officially labeled as a disease, for several reasons.
- “Obesity” doesn’t fit the definition of a medical disease. It has no symptoms, it’s not always harmful, and for some people in some circumstances, it may actually be protective.
- Many experts think “obesity” — the body efficiently storing calories as fat — is a normal adaptation to a set of circumstances (periods of famine) that’s held true for much of human history. Bodies that tend toward “obesity” aren’t diseased – they’re simply more efficient than naturally lean bodies.
- Medicalizing “obesity” could hurt patients by amplifying stigma around weight and pushing people into unnecessary and useless “treatments.”
There’s an excellent article in The Atlantic (“How obesity became a disease”) that discusses this and more.
Disclaimer: All information provided here is of a general nature and is furnished only for educational purposes. This information is not to be taken as medical or other health advice pertaining to an individual’s specific health or medical condition. You agree that the use of this information is at your own risk.
Hi, I’m Carrie Dennett, MPH, RDN, a weight-inclusive registered dietitian, nutrition therapist and body image counselor. I offer compassionate, individualized care for adolescents adults of all ages, shapes, sizes and genders who want to heal from an eating disorder, disordered eating or chronic dieting, cultivate an accepting, respectful relationship with their bodies, and gain the freedom to live an authentic, meaningful life without obsessing about food.
Need 1-on-1 help for your nutrition, eating, or body image concerns? Schedule a free 20-minute Discovery Call to talk about how I can help you and explore if we’re a good fit! I’m in-network with Regence BCBS, FirstChoice Health, Providence of Oregon Health Plan and United Healthcare, and can bill Blue Cross and/or Blue Shield insurances in many states. If I don’t take your insurance, I can help you seek reimbursement on your own. To learn more, explore my insurance and services areas page.
 Print This Post
Print This Post