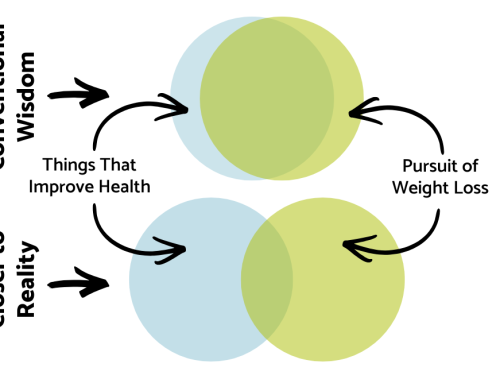
When it comes to health, does body mass index (BMI) matter? That question has been a matter of debate for decades. A mathematical formula originally developed by to look at trends in population health, today many healthcare providers use BMI as it was never intended—to diagnose individual patients.
Indeed, there are no shortage of health experts and non-experts (I call them trolls or busybodies) stating with an air of certainty that if you have a BMI of 30 or higher (“obese”), then you are going to die earlier than someone who has a BMI below 25 (“normal”). But you, dear reader, are not a statistic. As a society, we need to be focusing on behaviors that promote health and policies that promote health equity instead of placing so much focus on weight. Most weight talk really has little to do with health…sadly.
From the Quetelet Index to the BMI Index
The origin story of the BMI chart starts waaaaay back in 1835 with Lambert Adolphe Jacques Quetelet, a Belgian mathematician, astronomer, sociologist and statistician. He wanted an easy way to measure the degree of fatness in the general population, but the formula he came up with – weight in pounds divided by height in inches squared, then all of that multiplied by 703 – has no basis in human physiology.
In fact, not only did Quetelet manipulate the formula to try to match the data (which is very shoddy work), he explicitly said that his formula should not be used to gauge the level of fatness in an individual human. After all, he was not an expert on the human body, even to the limited extent we understood the human body back then.
Flash forward to 1972, and the Quetelet Index was rebooted as the Body Mass Index, with researchers converting numbers from those old Metropolitan Life Insurance Company height-weight tables into Quetelet’s formula. In the 1990s, the World Health Organization started using BMI, and it was off to the races.
But here’s the thing: a formula designed to assess the weight distribution of a population really isn’t good for anything else. It certainly can’t assess the health of an individual person. The idea that “underweight,” “normal weight,” “overweight” and “obese” are distinct categories and that slipping over the line from category to another by a mere decimal point means something for your health is B.S. Yes, BMI sounds scientific, but I’ve heard it referred to as mathematical snake oil.
To add insult to injury, that data used to develop the Quetelet formula and the MetLife tables is largely based on white people’s bodies, especially white male bodies. Not exactly representative of human diversity.

Think behaviors, not BMI
Even if you ignore the little “individual humans aren’t statistics” issue, there’s another problem. BMI can’t tell the difference between muscle, bone and fat — or where that fat is distributed in our bodies That’s huge, because maintaining muscle supports health, especially as we age. While excess body fat can increase the risk of chronic disease, but that largely depends on where that fat is located. Subcutaneous fat (fat under the skin) is thought to carry the least risk, while visceral fat (fat around the body’s abdominal organs) carries more risk, and fat deposits in the liver and muscles carry the most risk.
If you want to improve or maintain your health (and the health of others), then focusing on health-promoting behaviors and social justice is far more important than worrying about what BMI may or may not say about health.
While eating well and engaging in enjoyable physical activity are important, so is getting enough sleep, managing stress, staying socially connected and receiving preventive health care.
As for whether weight loss improves health, that depends. Research shows that for people who have BMIs in the “obese” range and have normal blood pressure, blood sugar and cholesterol levels, losing weight has not been shown to improve those biomarkers any further, and in some cases it actually contributes to unhealthy physical and psychological effects, including further weight gain.
One unfortunate finding of long-term research studies is that as many as half to two-thirds of healthy individuals who happen to be in the “obese” BMI range eventually become unhealthy in some way. (Of course, so do plenty of people in the “normal” BMI range.) While it’s not clear why this happens, increasing age and decreasing physical activity are likely factors…and so are weight stigma and socioeconomic status.
Stigma and low income (which may lead to living in less-than-safe neighborhoods that aren’t walkable) can be profound sources of stress. Stress contributes to the very health issues – chronic inflammation, high blood pressure, high blood sugar — that increase risk of cardiovascular disease and diabetes. Unfortunately, almost no studies looking at associations between weight and health actually assess for these important factors.

Keep on moving (and have fun with it)
Regular physical activity supports and improves health no matter what someone weighs. It also may also explain why having a higher weight doesn’t necessarily mean you’re going to get heart disease or diabetes (despite what many people believe).
Physical activity promotes stable blood sugar, blood pressure and cholesterol levels. It helps maintain or build lean muscle, improving body composition. The quality research studies that actually consider fitness when looking at the connection between weight and health tend to find that healthy “obese” individuals are fitter than their unhealthy “obese” peers. They also have essentially the same risk of chronic disease and premature death as the healthy “normal-weight” participants.
Physical activity doesn’t have to come from just gym workouts or other planned activity, either. Anything that gets you moving makes a difference. A 2015 study in the American Journal of Clinical Nutrition found that healthy higher weight individuals logged significantly more “incidental” activity — the type you get when you’re walking to the office water cooler or puttering around the house instead of sitting on the couch — than unhealthy higher weight individuals, but that moderate-to-vigorous physical activity was about the same between groups.

The bottom line (from my soapbox)
This is a HUGE topic, and I’ve really only scratched the surface her, but the important thing to remember – I’m going to say this one more time for the cheap seats in the back – is that individuals are not statistics.
Weight has become a handy-but-inaccurate shorthand for health. The truth is that having a lower BMI doesn’t automatically protect someone from developing health problems and having a higher BMI doesn’t guarantee that someone is unhealthy or will become so. No matter what statistics say, what’s important is your habits, your behaviors, your access to healthcare, and your feelings of connection and belonging in the world.
Disclaimer: All information provided here is of a general nature and is furnished only for educational purposes. This information is not to be taken as medical or other health advice pertaining to an individual’s specific health or medical condition. You agree that the use of this information is at your own risk.
Hi, I’m Carrie Dennett, MPH, RDN, a weight-inclusive registered dietitian, nutrition therapist and body image counselor. I offer compassionate, individualized care for adolescents adults of all ages, shapes, sizes and genders who want to heal from an eating disorder, disordered eating or chronic dieting, cultivate an accepting, respectful relationship with their bodies, and gain the freedom to live an authentic, meaningful life without obsessing about food.
Need 1-on-1 help for your nutrition, eating, or body image concerns? Schedule a free 20-minute Discovery Call to talk about how I can help you and explore if we’re a good fit! I’m in-network with Regence BCBS, FirstChoice Health, Providence of Oregon Health Plan and United Healthcare, and can bill Blue Cross and/or Blue Shield insurances in many states. If I don’t take your insurance, I can help you seek reimbursement on your own. To learn more, explore my insurance and services areas page.