Have you heard of the Semmelweis reflex? I hadn’t until I heard Evelyn Tribole, co-author of “Intuitive Eating” talk about it a few years ago. She actually mentioned it again when I interviewed her and Elyse Resch (her co-author) about the release of the 4th edition (and 25th anniversary edition) of their book.
So, if you’ve never heard of the Semmelweis reflex (also known as the Semmelweis effect), I certainly would not blame you! Let me explain what it is, then how it applies to Intuitive Eating, diet culture and weight stigma.
The misunderstood Ignaz Semmelweis
The Semmelweis reflex is a metaphor for the kneejerk, reflexive tendency to reject new evidence or knowledge because it contradicts existing, established beliefs or norms. It’s named after a real person, Hungarian physician Ignaz Semmelweis, who discovered in 1847 that deaths from what was commonly called childbed fever — bacterial infection of the female reproductive tract following childbirth or miscarriage — dropped dramatically when doctors disinfected their hands before moving from one person to another. Childbirth fever was a common problem in hospitals at the time, and often fatal.
Sounds reasonable, right? Especially given that the doctors were moving from dead people to pregnant women. In other words, doing an autopsy then immediately delivering a baby. Imagine you’re a pregnant woman in labor, and your doctor comes straight from having his bare hands in a corpse and then puts his bare hands, with whatever bacteria is on them, in your business? Not cool. And doctors’ maternity wards had three times the infection rates as midwives’ wards, because midwives weren’t performing autopsies.
Despite the fact that Semmelweis published his findings, which showed that handwashing reduced deaths from childbed fever to less than 1 percent, his observations were rejected by the medical community. This was partly because he couldn’t offer a scientific explanation for his observations (more on this in a moment), but also because doctors were offended at the very suggestion that they should wash their hands. Some simply refused to believe that a gentleman’s hands could transmit disease. Semmelweis was fired from the hospital, harassed by the medical community, and he eventually suffered a breakdown and died in an asylum.
It wasn’t until the 1860s and 70s, when Louis Pateur and other scientists developed the germ theory of disease, that there was finally an explanation for why hand washing mattered. Then, Dr. Semmelweis got the respect he deserved…even though he didn’t live to see it.

Belief perseverance
The Semmelweis reflex is a kissing cousin of “belief perseverance,” the psychological tendency to cling to discredited beliefs. That’s something we certainly see today. For example, some people still believe the Earth is flat, despite abundant evidence that firmly contradicts that belief.
Another such belief is that weight loss is essential for people who have body weights above the “normal” range on the body mass index (BMI) charts. This is certainly the dominant belief in the medical and scientific communities, and in our broader culture. Doctors are trained that they must prescribe weight loss for their larger-bodied patients, sometimes as the only “treatment” for a health issues when there are other, evidence-based, treatments available. For example, prescribing weight loss for knee pain when physical therapy is both evidence-based and more effective. Scientists doing research on the role of weight in health have trouble getting funding if their results don’t support the idea of weight loss.
Another example of this is when, in 2013, the American Medical Association decided to classify “obesity” (having a BMI of 30 or higher) as a disease requiring treatment and prevention, despite the fact that it’s own Council on Science and Public health concluded the year before that there wasn’t enough evidence to support this idea, and that calling “obesity” a disease wouldn’t help people be healthier. The AMA argued that this classification would help increase insurance reimbursement for weight loss drugs, surgery and treatment. (In other words, support the diet industry.)
The evidence says ‘A’, so let’s do ‘B’
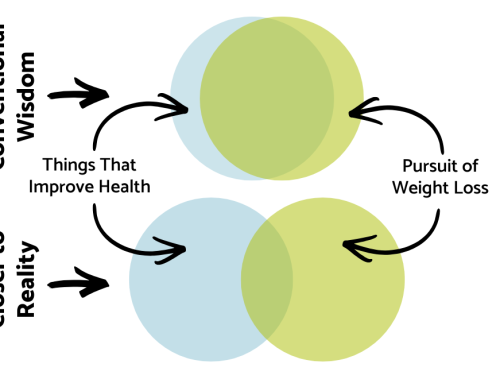
The AMA, and other entities that have also classified “obesity” as a disease, also claim that this will reduce weight stigma. In other words, instead of people in larger bodies being viewed as lazy or lacking in willpower, they will simply be viewed as someone with a disease. As diseased. Not only is that stigmatizing, it flies in the face of evidence that not all people with larger bodies are metabolically unhealthy, and not all people in thinner bodies are metabolically healthy. When I say “metabolically,” this loosely refers to blood pressure, cholesterol levels, blood sugar levels and chronic inflammation.
Even where there is evidence that being thin is associated with lower risks of certain health conditions, it’s a fact almost universally ignored that there is no evidence that people who are fat, and become thin, have the same lowered health risks as people who started out thin and stayed thin. So dieting to improve your health isn’t a slam-dunk, even if you are able to keep the weight off, which most people are unable to, another inconvenient fact.
I know a lot of researchers and doctors, and something I hear a lot is variations on this statement: “Yes, we know that most people who lose weight regain it, but we need to keep recommending weight loss.”
Why?

How stubbornness feeds weight stigma
The belief that “obesity” is a disease and that recommending weight loss is the answer perseveres in the face of growing research that weight stigma may cause many of the problems that are blamed on having “too much” body fat. People who experience and internalize weight stigma are more likely to suffer anxiety and depression, to avoid physical activity, to have disordered eating behaviors (including binging, purging, and risky weight loss attempts), to smoke, avoid preventive healthcare, and engage in other behaviors that pose health risks.
These effects of weight stigma? They’ve been observed in numerous studies across the BMI spectrum. In other words, if you have a “normal” BMI and have internalized the idea that you weigh too much and your body is wrong and needs shrinking, you may experience the same effects as someone is a much larger body who is told (and believes) that their body is wrong and needs shrinking. This is important, because part of the belief perseverance is pushback from “obesity experts” that the observed effects of weight stigma are actually due to weighing too much. They cling to the idea that body weight is a problem, even in the face of conflicting evidence.
Drilling down further, this pushback, this belief perseverance, happens in reaction to research showing that helping people adopt healthier behaviors (good nutrition, regular movement, body acceptance) without trying to shrink their bodies improves health. It also happens in reaction to research showing that people who score higher in intuitive eating traits (whether they come by them naturally, or because they’ve participated in intuitive eating counseling) have fewer disordered eating behaviors, better blood pressure and cholesterol levels, more varied diets, and better psychological health.
If it doesn’t work, do it anyway
This continued beating of the “obesity is a disease and we have to keep promoting weight loss” drum ignores the mounting evidence that weight does not equal health, and that the pursuit of weight loss itself causes harm. Interestingly, this drum-beating has become noticeably louder as the evidence against the intentional pursuit of weight loss mounts, a digging in of heels, if you will.
Why do people cling to old beliefs? In some cases money may be at stake, sure, but it’s also been suggested that the process of abandoning one of our convictions is a little like going through the grieving process. I certainly see that with individuals who are personally working on giving up the pursuit of dieting and the “thin ideal.” Definitely some grieving going on there, which is totally normal. It can be hard for chronic dieters (and doctors and scientists whose careers have been based on promoting weight loss) to accept that they invested so much time and effort on a fruitless quest at best, a harmful one at worst.
This is where self-compassion is really key. I say that from both personal and professional experience, as I first gave up my own pursuit of weight loss and accepted the idea that, based on the evidence, I could not ethically help my clients pursue weight loss.
I (and many dietitians an healthcare providers who come to similar realizations) went through a period of cognitive dissonance, where I simultaneously held the belief that the intentional pursuit of weight loss was futile and potentially harmful, and the belief that I still needed to try to help clients pursue weight loss if they desired it. This became increasingly stressful over time, to the point where I had to quit a job that I loved in many ways. This was a hard and messy process, and I am grateful that I allowed myself to experience the discomfort this brought up without becoming overwhelmed. Sort of swimming through the waves rather than letting them crash into me.
So, if you have been trying to let go of dieting and find it difficult, you’re not alone. Hopefully you know understand WHY it’s so difficult, and that understanding can free some headspace to hold competing beliefs in your head as you take the next steps in your journey. Not sure what that journey might look like? Let’s chat!
Disclaimer: All information provided here is of a general nature and is furnished only for educational purposes. This information is not to be taken as medical or other health advice pertaining to an individual’s specific health or medical condition. You agree that the use of this information is at your own risk.
Hi, I’m Carrie Dennett, MPH, RDN, a weight-inclusive registered dietitian, nutrition therapist and body image counselor. I offer compassionate, individualized care for adolescents adults of all ages, shapes, sizes and genders who want to heal from an eating disorder, disordered eating or chronic dieting, cultivate an accepting, respectful relationship with their bodies, and gain the freedom to live an authentic, meaningful life without obsessing about food.
Need 1-on-1 help for your nutrition, eating, or body image concerns? Schedule a free 20-minute Discovery Call to talk about how I can help you and explore if we’re a good fit! I’m in-network with Regence BCBS, FirstChoice Health, Providence of Oregon Health Plan and United Healthcare, and can bill Blue Cross and/or Blue Shield insurances in many states. If I don’t take your insurance, I can help you seek reimbursement on your own. To learn more, explore my insurance and services areas page.