You’re a grown-ass woman with decades of experiences to your credit, and you’ve got it all together — at least you look like you do. OK, sure, you never have a kind word for yourself when you look in the mirror, but who does, really? And, yeah, you’re obsessed with what you’re eating (or not eating), get anxious if you have to miss a planned exercise session, and maybe you indulge in some secret binges, and even an occasional purge? Those can’t possibly be signs of an eating disorder. After all, your friends, family and even your doctor praise you when you lose a few more pounds. Besides, you’re too “old” for an eating disorder…right?
Nope, you’re not too old. And you can absolutely develop a midlife eating disorder.
Looking beyond stereotypes
The stereotypical eating disorder patient is a white, female, high school or college student, but the truth is that eating disorders in midlife — and beyond — are all too common among women. (And while that’s the focus of this post, the reality is that eating disorders don’t “discriminate” based on gender, ethnicity, country of origin or skin color.)
A 2012 study estimated that 13 percent of American woman age 50 and older have eating disorder symptoms, higher than the rate of breast cancer. A 2017 study found that about 3.5 percent of women over 40 have a diagnosable eating disorder, yet most are not receiving treatment. Another 2017 study found that while rates of anorexia plateau around age 26, rates of bulimia plateau at around age 47, and rates of binge eating disorder don’t plateau until the 70s.
Awareness of eating disorders in midlife has been increasing slowly, in part because of psychologist Margo Maine’s 2005 book “The Body Myth.” Maine also authored the book “Pursuing Perfection.” When I’ve interviewed Maine previously, she told me that when she wrote “The Body Myth,” many of her adult eating disorder patients were mothers of former patients who finally realized that they had problems, too, in some cases hiding them for decades.

Midlife eating disorder triggers
Research suggests that most older women with eating disorders experienced at least some disordered eating — if not an actual eating disorder — early on in life. Basically, the seeds are planted early, then major life transitions later in life — divorce, illness, menopause, a child’s departure for college, an older parents’ health struggles — bring those seeds to fruition in the form of a resurgence of eating disorder symptoms, possibly more severe than what was experienced earlier in life.
Another possible trigger is the hormonal changes of perimenopause, which may open a “window of vulnerability” to developing eating disorders.
Given that today’s modern woman is likely to have a do-it-all, have-it-all mindset — perhaps coupled with perfectionism — and that’s a potent mix. It can be hard enough to take a break for some meaningful self-care by asking yourself “What do I need to do for myself today?” Taking time to ask yourself how you can stop dieting and develop a better relationship with food and your body? That’s even harder. It can feel easier to just jump on the next diet or exercise trend, trying to “fix” your body rather than befriending it while examining your thoughts, feelings and emotions.
Sadly, ageism may also be a trigger for midlife eating disorders, but it gets overlooked partly because of its subtlety. Not only does society encourage us to do whatever we can to be thin, it also encourages us to be forever young. This can lead women to engage in unhealthy eating and exercise practices to try to preserve the appearance of youth. But her lies the rub: looking younger may not translate to feeling younger, and that discrepancy between how we look and how we feel can also be distressing, triggering even more disordered eating behaviors.

Medical complications: worse with age?
While eating disorders don’t look much different in midlife than they do in adolescence or early adulthood, the effects and consequences can be very different. Eating disorders at any age take a toll on just about every body system, but older bodies are simply older, and may be more vulnerable to the medical complications of eating disorders.
Not only do eating disorders often accompany other mental health disorders, such as depression and anxiety, but they can harm digestive, bone, heart, reproductive and dental health. Some of these complications can lead to sudden death, as with cardiac arrest or suicide, or take a slower path, as with bone loss that leads to a hip fracture that leads to a downward health spiral. And then there’s quality of life — even if your eating disorders doesn’t kill you, it make your life less than what it could have been.

Why midlife eating disorders get missed
While eating disorders are underdiagnosed across the board, they’re missed more frequently in midlife. Women age 4o and older admitted for treatment at an eating disorder facility tend to have had their eating disorders longer than younger women who are admitted for treatment.
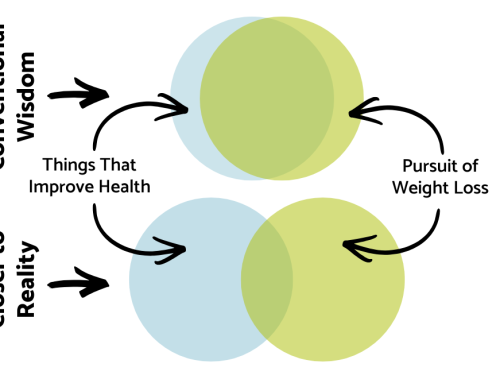
That’s partly because doctors have trouble seeing eating disorders in anyone other than young patients. Show up for your annual physical thinner than the year before, and you’re likely to be applauded rather than asked how you lost the weight, thanks to the healthcare system’s emphasis on weight as a standard of health. Not only can this contribute to weight stigma, it can also encourage eating disorders.
Speaking of weight stigma, that, along with shame, can be significant barriers to getting proper treatment for eating disorders. That’s because most people with eating disorders don’t live in visually emaciated bodies. Unfortunately, many people who are struggling with eating disorders while in larger bodies may actually be advised by their physician to eat less, exercise more, lose weight, making the situation even worse.
Maine told me she wrote “The Body Myth” after one of her patients, who had anorexia in college but developed bulimia after her second pregnancy, planned to open up to her doctor about her increasingly out of control symptoms, only to be greeted with “How does your husband like your new body?” when the doctor walked into the exam room. This makes me mad every time I think about it.

The bottom line
Eating disorders are always serious, and they don’t have to “look” a certain way in order to “count.” I can’t even tell you how many midlife clients I’ve had who struggle with, if not a diagnosable eating disorder, then very disordered eating behaviors. Often, the origins are in childhood or adolescence. This may include being put on a diet by your parents, being criticized about your weight or body, or growing up in a chaotic household where you controlled your food because it was the only thing you COULD control.
If you have concerns about some of your eating and exercise behaviors, or simply are interested in the topic, here’s some recommended reading (as an aside, I have interviewed all of these women before, and they are both extremely knowledgable and extremely compassionate, which I think is important):
- “The Body Myth: Adult Women and the Pressure to be Perfect” by Margo Maine, PhD
- “Pursuing Perfection: Eating Disorders, Body Myths and Women at Midlife and Beyond” by Margo Maine, PhD
- “Midlife Eating Disorders: Your Journey to Recovery” by Cynthia Bulik, PhD
- “Sick Enough: A Guide to the Medical Complications of Eating Disorders” by Jennifer Gaudiani, MD
This post contains Amazon Affiliate links. As an Amazon Associate I earn from qualifying purchases.
Disclaimer: All information provided here is of a general nature and is furnished only for educational purposes. This information is not to be taken as medical or other health advice pertaining to an individual’s specific health or medical condition. You agree that the use of this information is at your own risk.
Hi, I’m Carrie Dennett, MPH, RDN, a weight-inclusive registered dietitian, nutrition therapist and body image counselor. I offer compassionate, individualized care for adolescents adults of all ages, shapes, sizes and genders who want to heal from an eating disorder, disordered eating or chronic dieting, cultivate an accepting, respectful relationship with their bodies, and gain the freedom to live an authentic, meaningful life without obsessing about food.
Need 1-on-1 help for your nutrition, eating, or body image concerns? Schedule a free 20-minute Discovery Call to talk about how I can help you and explore if we’re a good fit! I’m in-network with Regence BCBS, FirstChoice Health, Providence of Oregon Health Plan and United Healthcare, and can bill Blue Cross and/or Blue Shield insurances in many states. If I don’t take your insurance, I can help you seek reimbursement on your own. To learn more, explore my insurance and services areas page.